Between constant emails and robust patient databases, interprofessional communication in healthcare is growing increasingly complex. A Sermo survey revealed that over 31% of providers feel ill-equipped to train staff in emerging technologies—but these technologies are central to modern healthcare communications. On top of this, physicians must navigate regulatory, economic, and cultural shifts, which all impact care coordination.
The result is a communication landscape that’s both high-stakes and fragile. When it works, multidisciplinary teams deliver safer, faster, and more satisfying care. When it breaks down, patients are harmed, physicians burn out, and clinical decisions are made on incomplete information.
This article is both a diagnosis of the communication problem and a practical toolkit for addressing it. It will examine the clinical evidence for why communication matters, identify the most common barriers—including ones physicians directly control—and walk through structured frameworks and strategies that individual physicians and care teams can put into practice today.
In this article, we’ll cover the current communications landscape, detailing barriers, methods and tips.

Why communication matters: the clinical evidence
About 68% of Sermo’s community of physicians communicate with other doctors at least once per week. The effectiveness of these conversations directly affects patient safety, clinical decision-making, and patient satisfaction.
Patient safety
Sermo polls report that 63% of patients rank their safety as the top priority when it comes to communication in healthcare—and physicians share this view. The Joint Commission attributes 60% of adverse events in hospitals to communication challenges. Similarly, researchers from the University of Bern and the University Hospital of Cologne associate poor communication with increased surgical complications and mortality rates.
Effective communication systems facilitate the urgency, accuracy, and clarity necessary to ensure patient safety. When structured communication tools are implemented, the results are measurable. One pre- and post-intervention study found that SBAR implementation reduced unexpected deaths from 0.99 to 0.34 per 1,000 admissions, demonstrating that structured communication tools can produce significant safety improvements when teams adopt them consistently.
Improved clinical decision-making
Information exchanges that involve all key stakeholders—including everyone from physician assistants to surgeons—contribute to improved clinical decision-making across the continuum of care.
On the role of multidisciplinary teams in effective decision-making, Adam Hetz, PA-C and Sermo member, noted: “As a physician assistant, I’ve witnessed firsthand the invaluable contributions that APPs make in filling critical gaps in care delivery. Our adaptability combined with our advanced training positions us to address emerging healthcare challenges and provide innovative solutions to meet the needs of our patients.”
When communication between healthcare professionals flows freely across disciplines, physicians gain access to clinical observations and contextual information that no single provider can capture alone. The alternative—siloed decision-making—means acting on incomplete data.
Improved job satisfaction
Physicians who have positive working relationships report higher rates of career satisfaction. This applies to both positive intra- and inter-professional relationships. The opposite is also true: care silos can make physicians feel overworked and undersupported.
Research consistently demonstrates that communication quality is one of the strongest predictors of professional fulfillment. When you feel that your clinical reasoning is understood and valued by the team around you, the work itself becomes more sustainable.
Improved patient satisfaction
The connection between effective communication and patient satisfaction extends beyond patient safety. It also strengthens continuity of care, providing emotional support, promoting treatment adherence, and fostering overall trust in healthcare providers.
As one Pediatrician and Sermo member put it: “Effective communication in healthcare provides good relationships and good teamwork and these help to improve patient satisfaction.”Patients who experience coordinated care, where their physician clearly communicates with specialists, nurses, and allied health professionals, are more likely to adhere to treatment plans and report higher satisfaction with their overall experience.
Interested in getting communication tips from fellow healthcare professionals? Connect with over 1 million physicians worldwide and share your experiences on the topics that matter to you.
“Effective communication in healthcare provides good relationships and good team work and these help to improve patient satisfaction.”
Sermo, Pediatrician

Barriers to communication in healthcare
Certain healthcare communication challenges are new. Others are a reflection of longstanding systemic issues. Understanding these barriers is the first step toward addressing them and many are within your sphere of influence as a physician.
Absence of integrated and compatible systems
A pressing, major healthcare challenge is bridging the two-way interoperability gap between medical apps and electronic health record (EHR) systems. Health IT systems are often incompatible with both internal and external systems, which can lead to underutilization and misuse. Non-interoperability also causes one-way communication and missed or delayed inclusion of allied health recommendations. Insufficient staff training further exacerbates this problem.
According to a Sermo survey of 100 U.S.-based healthcare leaders, 36% cited integration with their existing systems as an ongoing challenge, while 33% reported difficulties achieving interoperability with other healthcare facilities and networks.
Lack of values-based collaboration
According to one Sermo survey, APPs most often describe their working relationship with physicians as collaborative, supportive, and professional. Developing this type of collaboration is among the core communication skills for healthcare professionals. But coordination between medical professionals isn’t always streamlined. Communication gaps can occur for the following reasons:
- Different understandings of what “collaboration” means
- Omission of allied health input from discharge summaries
- Ambiguity in roles and responsibilities
- Limited direct time communicating with patients and reliance on junior staff for discharge
- Fragmented or incompatible technology systems
When asked how physicians could better support them day-to-day, 22% of APPs sought more collaboration in patient management, 19% wanted greater knowledge sharing, and 18% requested regular feedback on patient care—all of which require communication.
Hierarchical dynamics and psychological safety
Researchers from the University of Michigan associate breakdowns in healthcare communication with hierarchical gaps, reluctance to challenge authority, and role ambiguity. These factors can undermine the free flow of critical patient information and they deserve more than a passing mention, because they represent one of the most persistent and consequential communication barriers in medicine.
At the core of this issue is psychological safety: the shared belief within a team that it’s safe to raise concerns, ask questions, or point out errors without fear of punishment or humiliation. Research from the Agency for Healthcare Research and Quality (AHRQ) consistently shows that teams with high psychological safety communicate critical information more reliably and demonstrate better patient safety outcomes. Studies have found that psychologically safe environments improve the delivery of clinical care while simultaneously promoting job satisfaction and well-being among healthcare providers.
Here’s the uncomfortable truth for physicians: you typically sit at the top of the clinical hierarchy. How you respond when a nurse, resident, or PA raises a concern—whether with openness or dismissiveness—shapes whether the team communicates critical information in the future. A single dismissive response can silence a team member for months. The American College of Surgeons emphasizes that psychological safety in the OR, when combined with discipline and high expectations, leads to better outcomes, better problem-solving, and better psychological health for all members of the surgical team.
Communication during transitions of care
Care transitions such as shift changes, unit transfers, ED-to-inpatient, and discharge are the highest-risk moments for communication failure. Miscommunication during these handoffs contributes to about two-thirds of serious adverse events in hospitals, according to The Joint Commission, which identifies handoff failures as a leading cause of preventable adverse events.
The vulnerability is straightforward: providers finishing a shift may be fatigued and rushed, and more likely to omit key information important to a patient’s care. When information transfer is unstructured, critical details like pending lab results, conditional medication adjustments, and anticipated clinical changes can fall through the cracks.
The landmark I-PASS study published in the New England Journal of Medicine demonstrated that implementing a structured handoff protocol reduced medical errors by 23% and preventable adverse events by 30% across nine hospitals—with no increase in handoff duration. Handoff communication and patient safety are inseparable, and the evidence for structured approaches is now definitive.
Burnout and cognitive overload
Fatigued, cognitively overloaded physicians communicate less effectively resulting in shorter exchanges, reduced active listening, more missed information. The AHRQ identifies that work conditions such as time pressure, chaotic environments, and low control over work pace are strongly associated with physician burnout, which in turn threatens patient safety when depersonalization leads to poor interactions and when burned-out physicians suffer from impaired attention, memory, and executive function.
This creates a vicious cycle: documentation burden and communication inefficiency contribute to burnout, and burnout degrades the quality of communication. Time spent outside normal hours (often called “pajama time”) completing notes, orders, and reviews erodes the cognitive reserve physicians need to communicate effectively during clinical hours. Breaking this cycle requires both systemic support and individual strategies, which is why communication improvement and burnout prevention are deeply connected.
Absence of a dedicated care coordinator
Physicians often have heavy workloads that limit their available time to communicate comprehensively with inter- and intra-disciplinary care teams. This time constraint can result in missed or delayed information, which adversely affects patient care outcomes. That’s why multiple studies point to the need for a dedicated liaison—whether a social worker, nurse, or allied health professional—to bridge the gap between care teams.ial worker, nurse, or allied health professional—to bridge the gap between care teams.

Types of communication in healthcare
Collaboration is about more than formal meetings and verbal communication. Understanding the full landscape of communication methods helps you choose the right tool for each clinical situation.
Face-to-face
Face-to-face communication involves both in-person and remote video meetings or discussions. While the literature indicates that direct meetings are the most effective means of communication, it’s generally recognized as a secondary method because it’s less convenient.
Written
Written communication is currently the primary method of communication among physicians. Referral and discharge letters are the most common forms. The standardization and completeness of these documents directly impacts downstream care quality.
Email is less common because physicians cite concerns about privacy, security, and potential increases in workload. They also note its potential for medico-legal liability.
Structured electronic documents
Structured electronic documents are standardized and systematically include relevant patient information. While care teams benefit from their standardization, teams risk overlooking allied health input.
Shared EHRs
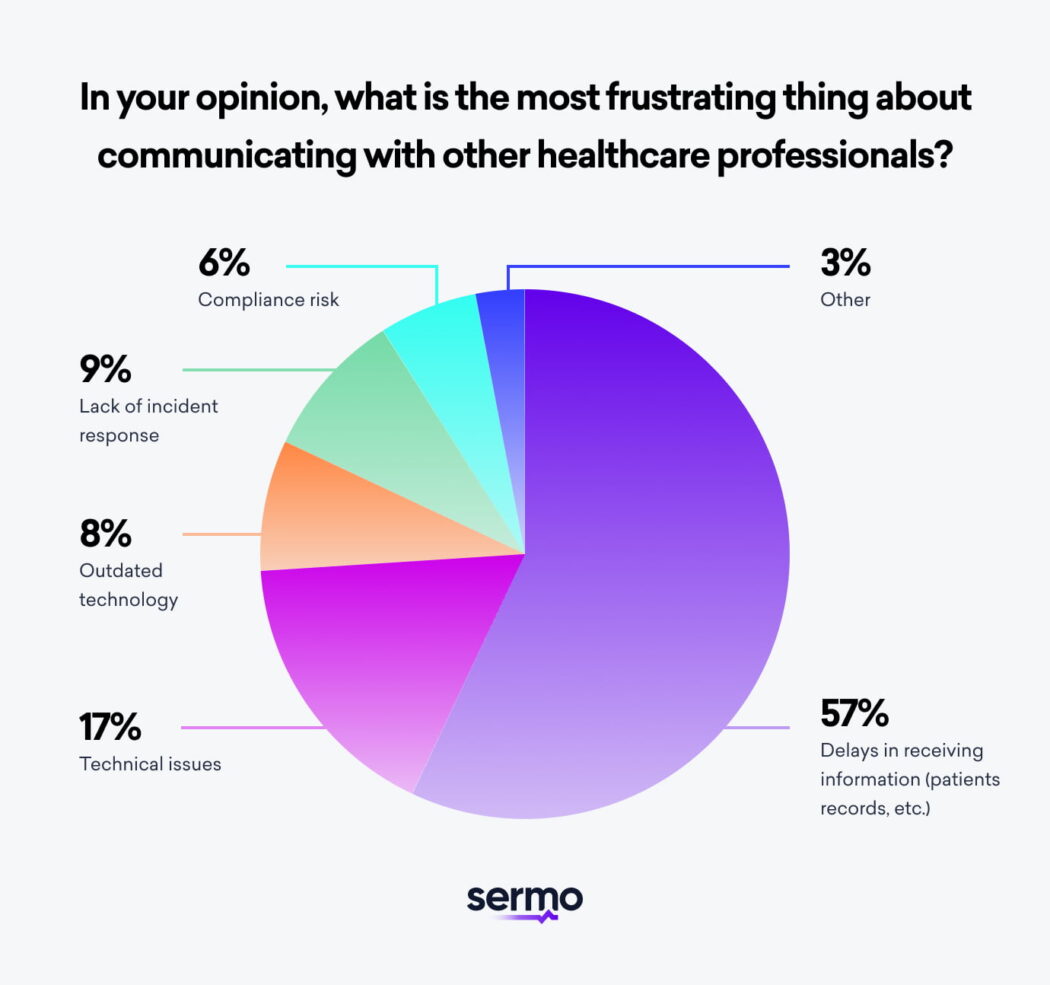
The majority of physicians use EHRs. Two-thirds (66%) of primary care physicians say they’re satisfied with their current EHR system, while 18% report strong satisfaction. Sermo asked physicians what the most frustrating part of communicating with other physicians is, and 57% reported delays in receiving information. EHRs’ capacity to reduce delays is effective, yet technologists are actively refining systems to improve interoperability. Improving interoperability remains a foremost industry priority.
Secure messaging and asynchronous platforms
HIPAA-compliant messaging platforms—such as TigerConnect, Voalte, and within-EHR messaging systems—are increasingly replacing pagers and phone calls for routine clinical communication. These platforms directly address the delay problem that 57% of Sermo members cite as the most frustrating communication barrier.
Unlike email, secure messaging platforms are designed for clinical workflows: they offer read receipts, priority flagging, role-based messaging, and integration with patient records. For non-urgent but time-sensitive communication, for example a consultant’s recommendation, a nursing concern that doesn’t warrant a phone call, or a pharmacy clarification, asynchronous messaging reduces interruptions while maintaining a documented communication trail.
The key for physicians is knowing when asynchronous communication is appropriate and when a direct conversation is needed. Routine updates and non-urgent clarifications work well asynchronously; deteriorating patients and complex clinical decisions require real-time dialogue.
Multidisciplinary team huddles
Brief, structured daily or shift-based standup meetings create a dedicated space for information exchange, flag high-risk patients, and reduce reliance on ad hoc communication. Huddles are one of the most effective low-tech communication interventions available.
A well-run huddle typically lasts 10–15 minutes, follows a consistent format (e.g., new admissions, high-risk patients, anticipated discharges, outstanding tasks), and includes representation from nursing, pharmacy, case management, and the physician team. The structure ensures that critical information surfaces proactively rather than reactively.
For physicians leading or participating in huddles, the key is consistency: showing up, listening actively, and responding to the information shared. When physicians engage meaningfully in huddles, it signals to the entire team that interprofessional communication is valued. reported difficulties achieving interoperability with other healthcare facilities and networks.
Practical strategies and frameworks for improving healthcare team communication
The barriers above are real, but they’re addressable. The following frameworks and strategies give physicians and care teams concrete tools to improve communication today, without waiting for institutional overhauls or new IT systems.
SBAR — the structured communication framework
SBAR stands for Situation, Background, Assessment, Recommendation—a structured communication framework originally developed by the U.S. Navy for nuclear submarine operations and adapted for healthcare in 2002 by Michael Leonard, MD, and colleagues at Kaiser Permanente.
Here’s how SBAR works in practice. Imagine a nurse calling you at 2 AM about a post-operative patient:
- Situation: “Dr. Chen, I’m calling about Mrs. Rivera in room 412. Her blood pressure has dropped to 82/54 and her heart rate is 112.”
- Background: “She had a right hemicolectomy 18 hours ago. Her last hemoglobin was 10.2 six hours ago. She’s received two liters of crystalloid since surgery.”
- Assessment: “I’m concerned she may be bleeding. Her drain output has increased and she’s become diaphoretic in the last 30 minutes.”
- Recommendation: “I’d like to get a stat hemoglobin, type and crossmatch two units, and have you come evaluate her.”
SBAR is endorsed by The Joint Commission, AHRQ, the Institute for Healthcare Improvement (IHI), and the World Health Organization (WHO). A systematic review published in BMJ Open found moderate evidence for improved patient safety through SBAR implementation, particularly when used to structure communication over the phone. One implementation study showed CIRS communication failures dropping from 31% to 11%, and unexpected deaths decreasing from 0.99 to 0.34 per 1,000 admissions.
SBAR works best for ad hoc communications. It gives both the sender and receiver a shared mental model for what information matters and in what order.
I-PASS — structured handoff for transitions of care
While SBAR handles ad hoc communications, I-PASS is designed specifically for structured shift-to-shift handoffs. The mnemonic stands for:
- I — Illness severity (stable, “watcher,” or unstable)
- P — Patient summary (brief clinical synopsis)
- A — Action list (to-do items and timeline)
- S — Situation awareness and contingency plans (“If ___ happens, then ___”)
- S — Synthesis by receiver (receiver summarizes and asks questions)
The landmark I-PASS study, published in the New England Journal of Medicine in 2014 and conducted across nine hospitals with over 10,000 patient admissions, demonstrated a 23% reduction in medical errors and a 30% reduction in preventable adverse events with no increase in handoff duration or negative impact on resident workflow. A subsequent multi-site study across 32 diverse hospitals found that adverse events were reduced by 47%.
I-PASS has the strongest evidence base of any handoff protocol. It is now recognized by AHRQ’s Patient Safety Network as the gold standard for effective clinical handoffs.
Understanding when to use which framework matters: SBAR is for ad hoc, event-driven communication. I-PASS is for structured transitions. Using the right framework in the right context maximizes the benefit of both.
Closed-loop communication
Closed-loop communication follows a simple three-step process: the sender communicates a message, the receiver repeats it back, and the sender confirms the repeat-back is accurate.
This technique is standard in aviation and the military, and it’s increasingly adopted in healthcare emergency and surgical environments. The American Heart Association and AHRQ’s TeamSTEPPS program both endorse closed-loop communication as a core team competency.
It takes seconds. It dramatically reduces verbal misunderstandings, particularly for medication orders, critical lab values, and procedure instructions. Consider the difference:
- Open loop: “Give 2 of epi.” → (Did they mean 2 mg? 0.2 mg? Epinephrine? Ephedrine?)
- Closed loop: “Push 1 mg of epinephrine IV now.” → “Pushing 1 mg of epinephrine IV now.” → “That’s correct.”
Closed-loop communication isn’t just for codes and emergencies. As the AHA TeamSTEPPS toolkit emphasizes: “Consider using it when providing any request in your daily practice to ensure everyone has a shared mental model.”
Building a speak-up culture
Frameworks like SBAR and I-PASS structure what information is communicated. But the most sophisticated framework is useless if team members don’t feel safe using it. Building a speak-up culture is the foundation on which all other communication improvements rest.
Practical steps for physicians:
- Explicitly invite input. Instead of “Any questions?” (which rarely generates responses), try: “What concerns do you have about this plan?” or “What am I missing?”
- Respond non-defensively when challenged. When a nurse or resident questions your order, your response in that moment teaches the entire team whether speaking up is safe. A simple “Good catch—let me reconsider” or “Walk me through your concern” goes further than any institutional initiative.
- Model the behavior. Speak up when you identify potential issues in another team member’s domain. When physicians demonstrate that cross-disciplinary input is welcome, it normalizes the behavior for everyone.
The Sermo APP data reinforces the demand for this culture: 22% want more collaboration, 19% knowledge sharing, and 18% regular feedback—all of which require an environment where speaking up is safe.
Ensure data liquidity
Prioritize systems that export patient data in widely accepted standardized formats, like CCD/C-CDA, and integrate external data. This lets you create and maintain comprehensive, longitudinal patient records. When data flows freely between systems, you spend less time hunting for information and more time making clinical decisions.
Prioritize data security
Compliance risks and technical issues are core communication problems—both of which concern sensitive patient data. Practice leaders or owners can increase the security of your communications systems through:
- Physical safeguards: Install high-definition security cameras at all access points, restrict entry to server rooms with biometric or keycard systems, and use backup generators to maintain uptime.
- Administrative safeguards: Develop and enforce comprehensive data handling policies, provide regular training to employees on compliance, and appoint a Chief Information Security Officer.
- Technical safeguards: Deploy robust firewalls and encryption protocols, implement network address translation to conceal internal IP addresses, and enforce multi-factor authentication (MFA).
Support team-based care
Many EHRs don’t allow team members to enter data or perform tasks in accordance with their licensure or privileges. If you have the ability to influence your practice environment, advocate for EHR configurations that allow all key stakeholders to directly contribute information to the record.
In supporting team-based care, consider how hierarchies impact collaboration and patient care outcomes. When APPs, nurses, and pharmacists can document directly in the shared record rather than relaying information through intermediaries, communication becomes faster, more accurate, and less prone to the “telephone game” effect that plagues fragmented workflows.
How technology is reshaping healthcare communication
Technology is both the source of many communication challenges and the most promising avenue for addressing them. Understanding what’s working, what’s emerging, and what to watch out for helps physicians navigate this rapidly evolving landscape.
AI-powered communication tools
Ambient AI scribes represent perhaps the most significant recent technology shift in physician communication. These tools use machine learning to transcribe and summarize patient-physician conversations in real time, freeing physicians from the keyboard during clinical encounters. The Permanente Medical Group’s deployment of ambient AI scribes across 10,000 physicians and more than 2.5 million patient encounters found an estimated 15,791 hours of documentation time saved—the equivalent of 1,794 eight-hour workdays—while improving patient-physician interactions and physician satisfaction.
A multi-site study published in JAMA found that AI scribes were associated with daily reductions of 13 minutes in EHR usage and 16 minutes in documentation time. While these are modest numbers, the impact on burnout reduction appears to exceed what the time savings alone would predict—suggesting that the qualitative shift in how physicians experience their clinical encounters matters as much as the quantitative time saved.
Beyond ambient scribes, AI is also being applied to generate clinical summaries for handoffs, create smart alert systems that prioritize critical information, and flag communication gaps in care transitions.
Interoperability progress and gaps
FHIR (Fast Healthcare Interoperability Resources) has emerged as the global standard for healthcare data exchange. Built on modern web technologies, FHIR is making it progressively easier for systems to share patient data. In 2025, 71% of countries surveyed report active FHIR usage, with 54% of stakeholders expecting strong adoption growth—up from 39% the year prior.
Yet the cross-institutional communication challenge that Sermo members identify persists: 36% cite system integration challenges, and 33% report inter-facility interoperability difficulties. Health information exchanges and standards like TEFCA (Trusted Exchange Framework and Common Agreement) are making progress, but true seamless data sharing between unaffiliated health systems remains a work in progress.
For individual physicians, the practical takeaway is to advocate for interoperable systems when you have influence over technology decisions, and to develop workarounds like structured verbal summaries, standardized referral templates, and direct phone calls when the technology falls short.
The double-edged nature of technology
Technology that reduces delays can simultaneously create alert fatigue and over-reliance on asynchronous messaging. When every notification is flagged as urgent, nothing feels urgent. When every communication is routed through a messaging platform, the nuance that comes from direct conversation is lost.
EHR “pajama time” competes directly with the cognitive recovery physicians need to communicate effectively. As ambient AI scribes and other tools mature, their potential to reduce this after-hours burden could indirectly improve communication quality by preserving cognitive capacity for clinical interactions.
The lesson for physicians: technology is a tool, not a solution. The most effective communicators use technology to handle routine information transfer while preserving direct, real-time communication for complex clinical discussions and relationship building.
Join a global network of physicians
Sermo surveyed its community of physicians to learn what motivated them to pursue medicine. Almost half (46%) said, “I just wanted to help others.” But communication challenges can inhibit physicians’ ability to serve their local community.
That’s why it’s beneficial to join a network of physicians who share your challenges and concerns. Learn how other physicians approach interprofessional communications, discuss strategies that work, and find peer support for the challenges that don’t have easy answers.
As one Sermo member from Colombia put it: “I got a lot of help from colleagues from all around the world, it was very amazing.”
Sermo is the largest global online platform where doctors connect on the topics that matter to them and their patients—and have a few laughs along the way. Become a Sermo member today.
Key takeaway
Communication failures in healthcare are systemic, measurable, and—critically—addressable with structured tools and deliberate practice. The evidence is clear: frameworks like SBAR and I-PASS reduce errors and save lives. Closed-loop communication eliminates misunderstandings that take seconds to prevent but can take days or weeks to repair. And the culture you create on your team may be the single most impactful communication variable you control.
None of this requires institutional approval, IT procurement, or policy redesign. It requires a physician who decides that communication is a clinical skill worth investing in, just like any other. Physicians who adopt structured frameworks, build speak-up cultures on their teams, and engage with peers on communication challenges are investing in both patient safety and their own professional satisfaction. Join the conversation on Sermo.